Diabetes Mellitus and the Power of Exercise in Disease Management
By Nicole Vanderschaaf
March 11, 2026
Have you ever noticed how you feel instantly energized after eating a meal, or how your bad mood suddenly disappears once you grab a snack? It’s almost like flipping a switch, right?
Have you ever noticed how you feel instantly energized after eating a meal, or how your bad mood suddenly disappears once you grab a snack? It’s almost like flipping a switch, right? That boost in energy is no coincidence—it comes from the way your body breaks down the food you eat and converts it into energy. Behind that familiar feeling is a finely tuned system that regulates your blood sugar and keeps your cells energized. But what happens when that system stops working properly and your body can’t use that energy effectively? That’s where diabetes begins. In this article, we will first explain the physiology behind diabetes mellitus and then explore how physical activity supports diabetes care.
The physiology behind Diabetes Mellitus
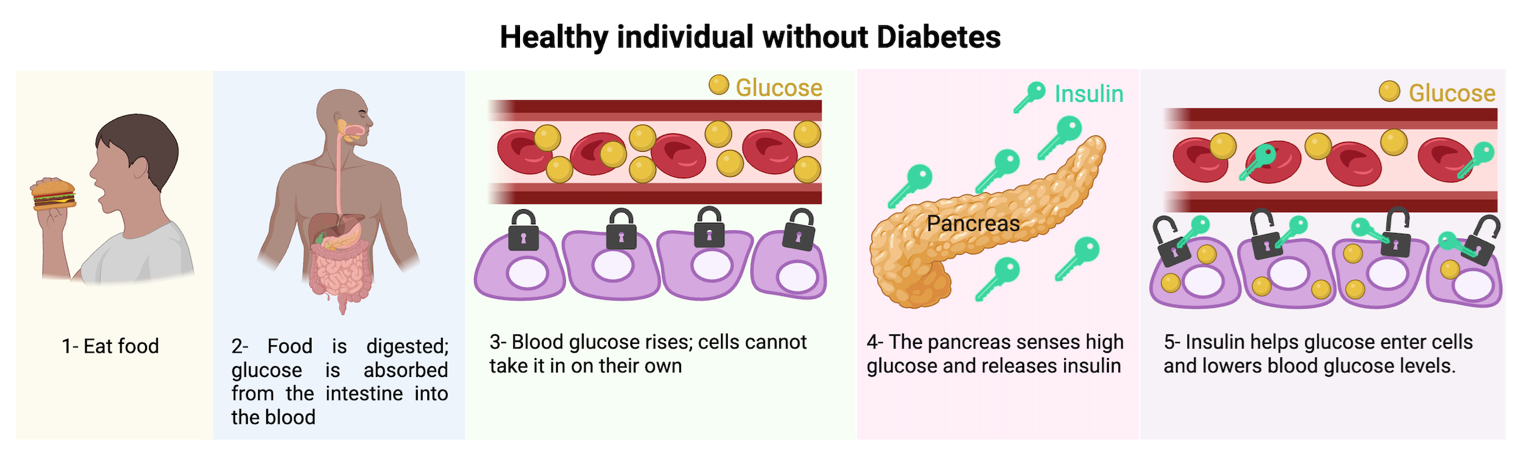
Food is an essential part of our daily lives, as it provides our bodies with the energy we need to move and function properly. Much of that energy comes from carbohydrates like glucose or more commonly named “sugars” in food, which enter the bloodstream after digestion. Once in the blood, the pancreas senses the increase in glucose levels and releases a hormone called insulin. In a healthy individual, insulin acts like a key that opens the doors of the cells, allowing glucose to enter and be used for energy, while lowering glucose levels in the bloodstream (Fig. 1). In individuals with diabetes, the body either does not produce enough insulin (Type 1 and Type 2 diabetes) or cannot effectively use the insulin it secretes (Type 2 diabetes). As a result, the cells do not receive the “key” needed to open the door and allow glucose to enter, so glucose remains in the bloodstream. This is why high blood glucose levels are a characteristic feature of diabetes 1,2,3.

Figure 1. Normal regulation of blood glucose in individuals without diabetes.
In individuals with diabetes, cells aren't getting enough energy to function properly, even though plenty of sugar is available. This often leads to fatigue and a significant decrease in energy. Moreover, this buildup of sugar in the blood begins to harm blood vessels, making them stiff and irritated. Over time, this increase in blood sugar can harm major organs such as the heart and kidneys, as well as other organs.
Where is insulin produced? Diabetes often stems from an issue with the pancreas, which is a large fish-shaped gland located in the back of your abdomen, just behind your stomach. When your blood sugar increases, the pancreas, specifically the beta-cells in pancreatic islets, sense the increase and secrete insulin to lower sugars back to a healthy level 2. In diabetes, the production or usage of insulin is heavily impacted, meaning the body can’t lower its blood sugar back to a healthy level after eating a meal.
What is the difference between Type 1 vs Type 2 Diabetes? Type 1 diabetes is an autoimmune disorder where your immune system falsely recognizes beta-cells (the ones that secrete insulin) in the pancreas as dangerous and attacks and destroys them 2,3. This leads to a significant drop in the production and secretion of insulin in the body. In individuals with Type 1 diabetes, cells do not receive the “key” they need to take in glucose, so glucose remains in the bloodstream. As a result, the body cannot effectively use the sugar from food for energy, leading to high blood glucose levels and the need for external insulin administration (Fig. 2).
Type 2 diabetes is the most common form of diabetes and is associated with both reduced insulin secretion and impaired cellular response to insulin. In this scenario, cells may not receive enough insulin, or they respond poorly to the insulin that is present (the “key” no longer works effectively) 1,2,3. When the “key” does not work properly, this is called insulin resistance. Due to the complexity of Type 2 diabetes, management is more complicated than simply administering insulin (Fig. 2).
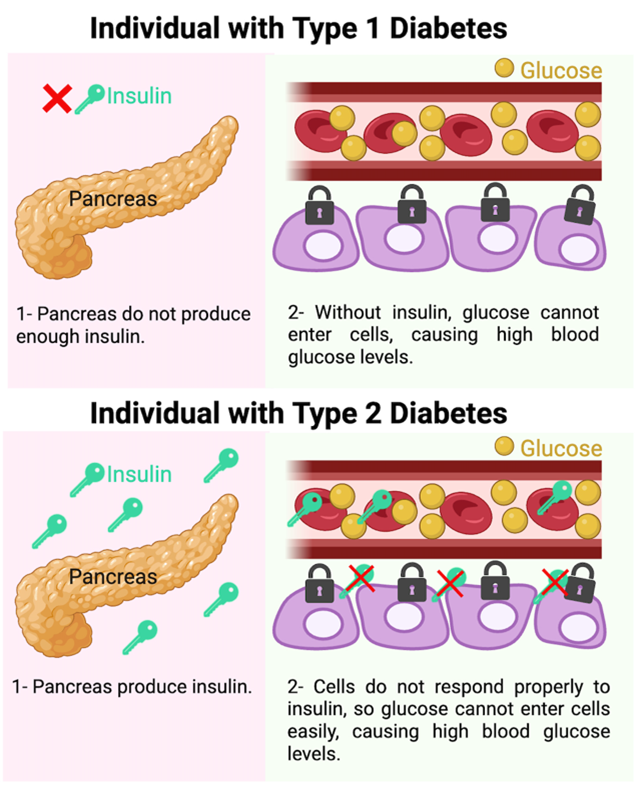
Figure 2. Key differences between type 1 and type 2 diabetes mellitus.
What are the common symptoms of diabetes if it’s not managed? One of the most common symptoms associated with diabetes is fatigue or low energy. It is important to note that fatigue is not the same as being tired. A tired person may feel significantly better after resting, but for individuals with persistent fatigue, resting does very little to help4. Diabetes disrupts the body’s ability to use insulin to move glucose from the blood into cells, leaving cells without the energy they need. As a result, the body remains in a state of low energy.
Another very common symptom seen in patients with diabetes is increased thirst and urination 4. In a healthy individual, the kidneys play a vital role in removing waste while retaining essential nutrients like glucose. However, when blood glucose levels become too high, as in diabetes, the kidneys cannot keep up. As a result, they reach a “reabsorption limit,” and excess glucose spills into the urine. This is why glucose can be detected in the urine of individuals with diabetes. When glucose enters the urine, it draws water along with it through a process called osmosis, leading to increased urine production. Consequently, the body loses more water than normal. In response, the brain senses this water loss and triggers intense thirst to encourage water intake and restore fluid balance.
Physical activity: A Powerful Tool Against Diabetes Mellitus
Regular physical activity is a key for managing diabetes. When you exercise, the demand on your muscles increases and, their demand for energy increases. Because of this, exercise promotes the movement of proteins called GLUT-4 transporters in body cells. It’s like exercise opens the doors of the cells, allowing glucose to enter without needing the “key” (insulin).
Exercise also helps cells to response to insulin signals. Over time, the muscles become more sensitive to insulin, and our muscles become more efficient at utilizing glucose (Fig. 3) 5,6. Exercise helps lower high blood glucose levels independently of insulin—a major benefit for both healthy individuals and those with diabetes.
In addition to these immediate effects, regular physical activity can improve overall insulin sensitivity, support cardiovascular health, and help maintain a healthy body weight. Exercise is often recommended as part of a comprehensive diabetes management plan because it addresses both blood glucose control and long-term health outcomes.
It is important to note that individuals with diabetes should monitor their blood glucose levels and consult with a healthcare professional before beginning a new exercise program, especially if their diabetes is not well controlled. When done safely and consistently, physical activity serves as a powerful, non-pharmacological tool in diabetes care.
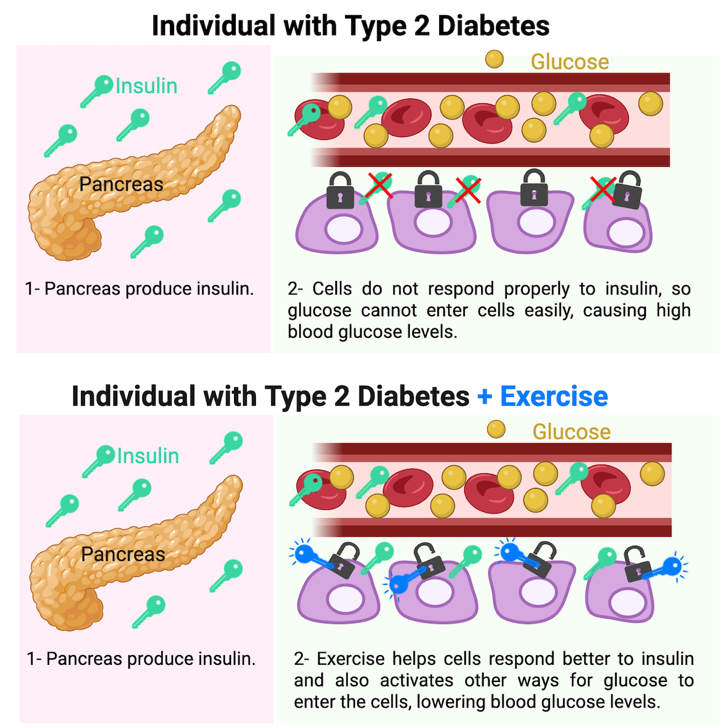
Figure 3. Exercise is a crucial, non-pharmacological component of diabetes management.
Summary
In summary, diabetes is a complex condition that disrupts the body’s ability to regulate blood sugar. The good news is that regular physical activity can help improve blood glucose control and support long-term health in both healthy individuals and those with diabetes. However, people with diabetes should take precautions and work closely with a healthcare professional to tailor an exercise plan that is safe and effective.
Acknowledgment
Nicole Vanderschaaf is a Doctor of Physical Therapy student at ISU. This article is the result of a research literature project led by Dr. Lizbeth de la Cruz (Biological Sciences). It was edited, reviewed, and prepared with additional contributions from Dr. Sherry Adams (Biological Sciences) and Tarang Jain (Physical Therapy and Athletic Training). Logan McDougall and Bentley Parrott provided feedback to strengthen the writing. Figures were created by BioRender.
References
- 1. Lu et al, Type 2 diabetes mellitus in adults: pathogenesis, prevention and therapy. Signal Transduct Target Ther, 2024. DOI: 10.1038/s41392-024-01951-9
- 2. Britannica Editors. Diabetes mellitus 2026. https://www.britannica.com/science/diabetes-mellitus
- 3. Banday MZ, et al, Pathophysiology of diabetes: An overview. Avicenna J Med. 2020. DOI: 10.4103/ajm.ajm_53_20
- 4. Kalra S and Sahay R. Diabetes fatigue syndrome. Diabetes Ther. 2018. DOI: 10.1007/s13300-018-0453-x
- 5. Riddell M and Perkins BA. Exercise and Glucose Metabolism in Persons with Diabetes Mellitus: Perspectives on the Role for Continuous Glucose Monitoring. J Diabetes Sci Technol, 2009. DOI: 10.1177/1932296809003004396.
- 6. Chipkin SR et al, Exercise and Diabetes, Cardiology Clinics, 2001. https://doi.org/10.1016/S0733-8651(05)70231-9
