Advanced Surgical Obstetrical Training
You thought the country doctor delivering babies was quaint history?
At ISU Family Medicine Residency, we train all residents for full spectrum rural Family Medicine, which includes continuity deliveries and more-than-average time on Labor & Delivery.
Some of our residents know they want to practice in more remote rural places where they will not only have OB as a large part of their practice, but they also need to be trained to be their own surgical back up, meaning they will need to be able to deliver babies by Cesarean Section.
Curriculum
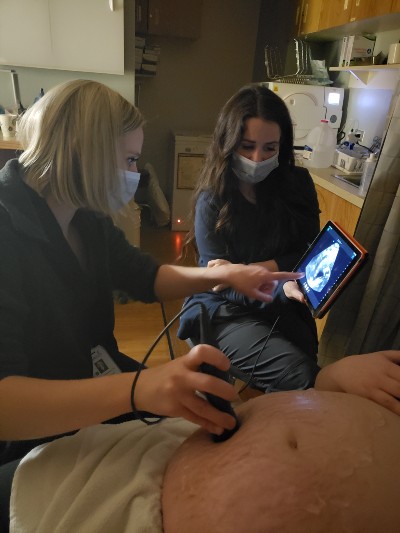
Near the end of the R1 year, interested residents can apply to Advanced Surgical Obstetrical Training Track. R2s and R3s in ASOTT attend quarterly small-group didactics on topics such as surgical anatomy, instrumentation, managing complications, surgical anesthesia, tubal ligation, hysterectomy, and OB ultrasound. ASOTT residents are also given preference to attend C-sections and are assigned more continuity patients.
OB Numbers
Over the last five years ASOTT residents have averaged 160+ vaginal deliveries and 40+ C-sections upon graduation, equipping them to be privileged in surgical OB in rural hospitals, providing essential obstetrical care in underserved areas.
Wilderness Medicine

Many rural physicians choose to live in remote places because they also enjoy playing in their backyard: hiking, camping, hunting, skiing, biking, climbing, etc.
Intentionally or unintentionally, they often render first aid to friends, family, and strangers met upon the trail. Wouldn’t you prefer to be equipped for that situation when it arises?
All ISU FMR residents are invited to participate in the Wilderness Medicine didactics offered at our summer & winter retreats and routine noon lectures. R2s or R3s with a significant interest in Wilderness Medicine can choose to participate in WMAOC.
This will include:
- Volunteering with the Pebble Creek Ski Patrol
- Obtaining certification in Advanced Wilderness Life Support
- Attend a mountain rescue and transport course
- Presenting Wilderness Medicine didactics.

Lifestyle Medicine

Lifestyle Medicine is evidence-based medicine, using therapeutic lifestyle interventions to prevent, reverse, and treat non-communicable chronic conditions.
Upon completion of Lifestyle Medicine Track requirements, residents are qualified to sit for the American Board of Lifestyle Medicine Certification.
Curriculum
6 Pillars of Lifestyle Medicine:
- A whole-food, plant-predominant eating pattern
- Physical activity
- Restorative sleep
- Stress management
- Avoidance of risky substances
- Positive social connections
Physician Tools for Patient Care:
- Motivational interviewing, assessing readiness for healthy lifestyle changes
- Assist patients in creating SMART goals
- Write nutrition and exercise prescriptions
- Role model a budget-friendly, healthy lifestyle to our communities
Outcome: American Board of Lifestyle Medicine certified physicians (DipABLM) carry the benefits of lifestyle medicine into their communities and assist in mitigating the root causes of chronic conditions. This in turn leads to the development of healthier and happier communities.


